
1. Definition and Purpose
Euthanasia is derived from the Greek terms eu (good) and thanatos (death), meaning “a good death.” It refers to the act of ending an animal’s life in a manner that minimizes or eliminates pain, fear, and distress.
From a One Health perspective, humane euthanasia not only protects animal welfare but also promotes public health, human psychological well-being, and environmental safety. Each decision to euthanize should be grounded in compassion, respect, and cultural awareness.
2. Guiding Principles
When euthanasia is deemed necessary, it must be performed with the highest degree of respect and minimal distress to the animal.
In situations where preferred agents or methods are unavailable, it may still be considered humane to use an alternative method promptly to end suffering rather than delay euthanasia or transport an animal in pain.
Four essential criteria for humane euthanasia:
- Minimize pain and discomfort.
- Achieve rapid unconsciousness.
- Minimize fear and distress.
- Ensure the process is reliable and irreversible.
3. Client Consent and Authorization
Obtaining informed client consent is an essential part of the euthanasia process. It ensures that the client fully understands the reasons for euthanasia, the procedure, and what will happen afterward. It also provides legal and ethical documentation of owner authorization.
Steps for obtaining consent:
- Discuss the rationale for euthanasia clearly and compassionately, including the prognosis, quality-of-life concerns, and alternatives (if any).
- Describe the procedure in plain language, including what the client may observe (e.g., brief movements after death).
- Discuss remains handling (burial, cremation, or community disposal protocols) and confirm the client’s wishes.
- Provide emotional support—clients may need time to process the decision.
- Obtain written consent using the designated Euthanasia Consent Form, signed by the owner (or authorized agent) and a staff witness.
Documentation requirements:
- Date and time of consent.
- Name and signature of owner/agent.
- Animal identification details (species, name, description).
- Method of euthanasia.
- Staff or veterinarian signature and credentials.
In remote or emergency field conditions where written consent is impractical:
- Obtain verbal consent in the presence of at least one staff witness.
- Record the interaction in the medical or field record, noting time, date, names, and reason for verbal consent.
- Follow up with written documentation as soon as possible.
Maintaining proper consent records demonstrates transparency, builds community trust, and upholds professional and legal standards.
4. Handling and Preparation
- For tame or socialized animals, use gentle restraint, calm tones, and familiar surroundings when possible. Sedation should always be provided before euthanasia.
- Available sedatives will include oral trazadone and gabapentin to be given ahead of time if applicable and injectable medetomidine, butorphanol, hydromorphone, acepromazine, ketamine, and valium – the veterinarian performing the euthanasia may choose the protocol they prefer with the drugs provided at the remote clinic.
- All drugs used must be appropriately logged.
- For fearful, feral, or aggressive animals, minimize handling to reduce distress and risk to staff.
- If you can, try to give gabapentin and trazadone hidden in food ahead of trying to sedate the animal.
- Use a tranquilizer pole to inject sedatives into the pet if unable to safely handle.
- Limit visual, auditory, and tactile stimuli.
- Covering the animal with a blanket or towel can help calm it and enhance safety.
- Always prioritize staff safety and animal welfare.
5. Acceptable Methods of Euthanasia
5.1 Injectable Barbiturates (Preferred Method)
- Pentobarbital sodium, administered intravenously by a licensed veterinarian following sedation, is the preferred and most humane method.
- Intraperitoneal (IP) or intracardiac (IC) injection is acceptable only if the animal is unconscious or under deep sedation.
- IP injection is acceptable for small animals or neonates where venous access is not possible.
- Proper administration results in rapid unconsciousness, respiratory arrest, and cardiac arrest.
- Amount of euthanasia solution must be logged in appropriate drug log.
5.2 Firearms (Alternative Method in Remote Areas)
While distressing for many, proper firearm use can be a humane and practical alternative in communities where chemical agents or veterinarians are unavailable. This section is not intended to say that staff of One Health remote clinics would be performing euthanasia via firearms. It is written to illustrate what we deem an acceptable protocol for communities to have when no veterinary team is accessible, and they have an animal in distress that needs immediate euthanasia.
Key considerations:
- Only trained, licensed individuals may perform firearm euthanasia.
- Local law enforcement (e.g., RCMP) should be notified or present when possible.
- Always consider safety of personnel, bystanders, and other animals.
- Conduct outdoors, in a secure area with a safe backstop and no public access.
- Sedate the animal beforehand whenever feasible. Check with the local nursing station to see if they have gabapentin and/or trazadone that they can dispense at a dose of 40 mg/kg for gabapentin and 10mg/kg for trazadone. Estimate the weight to the best of your ability and round up your doses. Always best to give more sedation than not enough. Plan accordingly, as it may take up to an hour or more after ingestion before effects are seen. Arrangements can be made for medetomidine to be provided by the Winnipeg Humane Society if there is a trained individual in the community that is able to give IM or SQ injections. An appropriate dosing chart will be provided. The medetomidine may be kept in the community and a protocol will be developed for its safe storage based on the unique circumstances of each community.
Technique:
Dogs:
- If the dog is not immobilized by sedation, it should be fed some food from an elevated position to raise the head to a height that is easy to aim at. Alternatively, the dog can be tethered in position, but a person should not restrain the animal.
- Aim midway between the eyes and the base of the ears, slightly off-center to avoid the skull ridge.
- The shot should be directed slightly across the head and toward the spine.
- Always ensure a safe backdrop (e.g., soil berm).
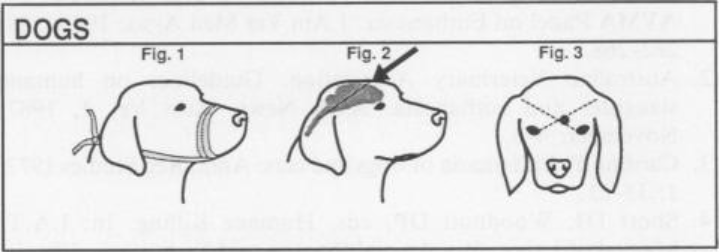
Cats:
- Always sedate first as they are much harder to euthanize with this method. Immobilization with medetomidine is preferred.
- Wrap in a towel or blanket with only the head exposed or contain in a box. A person should not restrain the cat.
- Aim at the center of the forehead slightly below an imaginary line between the ears.

When properly performed, unconsciousness is immediate and irreversible. Reflex muscle movements (convulsions) may occur and should not be mistaken for consciousness.
6. Confirmation of Death
Death must always be verified before carcass handling or disposal. Use multiple indicators:
- Absence of breathing – Observe for 1–3 minutes.
- Absence of heartbeat – Feel or auscult over the chest.
- Absence of corneal (blink) reflex – Touch the surface of the open eye; no blink reflex should occur.
- Fixed, dilated pupils.
- Rigor mortis – If in doubt, wait until rigor mortis is evident before disposal.
7. Carcass Disposal
- Confirm death before disposal.
- All carcasses should be disposed of within 48 hours in accordance with local, provincial, and federal regulations.
- Carcasses euthanized using barbiturates must be buried or incinerated—these substances remain toxic to wildlife and scavengers.
- Deep burial (at least 4 ft / 1.2 m) in a secure, non-flooding area is preferred.
- If burial is not possible (e.g., frozen ground), store carcasses securely until proper disposal is possible.
- Proper carcass management also prevents disease transmission and protects community and environmental health.
8. Documentation and Record-Keeping
Accurate records are critical for accountability, transparency, and monitoring. Record the following:
- Date, time, and location of euthanasia.
- Species, description, and identification (if applicable).
- Reason for euthanasia.
- Method and dose of agent used.
- Sedation details.
- Names and roles of personnel involved.
- Carcass disposal method and location.
Records should be stored securely and made available for veterinary or regulatory review upon request.
9. Cultural and Community Sensitivity
Respect for cultural perspectives surrounding animals, death, and disposal practices is essential.
- Engage community leaders and local authorities whenever possible.
- Provide clear explanations of the procedure and rationale.
- Avoid performing euthanasia in public or in view of other animals.
- Provide emotional support and debriefing for staff and community members involved.

10. Staff Safety and Wellbeing
Performing euthanasia can have emotional and psychological impacts.
- Encourage team debriefing and access to mental health resources.
- Ensure staff never work alone during euthanasia procedures.
- Provide training and refreshers on humane handling, firearm safety, and compassion fatigue management.
